Unfinished business: The first step to aged care reform in Australia

One element of the current Government’s plan to reform the aged care system in Australia has been introduced into Parliament – the Royal Commission Response Bill – with more to follow.
On 1 March 2021, the Royal Commission into Aged Care Quality and Safety tabled its final report in Parliament. The Royal Commission was established in October of 2018 and released its Report just shy of 2.5 years later, calling for an overhaul to the aged care industry and painting a “gloomy” picture of the state of the system. With no less than 148 recommendations, the Report failed to outline a clear path to reform, instead providing the Government with the flexibility to cherry-pick recommendations best suited to its policy objectives.
After a long period of regulatory uncertainty, the aged care industry keenly awaited the Coalition Government’s response to the findings. This came with two Bills, one which was passed and another which lapsed upon the calling of the election. As proposed aged care reforms headlined the current Government’s 2022 campaign strategy, all eyes were on Labor’s Aged Care and Other Legislation Amendment (Royal Commission Response) Bill 2022 (Royal Commission Response Bill). This was a reiteration of the Coalition’s second bill of 2021, adopting only 9 of the 148 recommendations. Albeit a step in the right direction, this Bill signifies that the reform of Australia’s aged care system is still very much unfinished business.
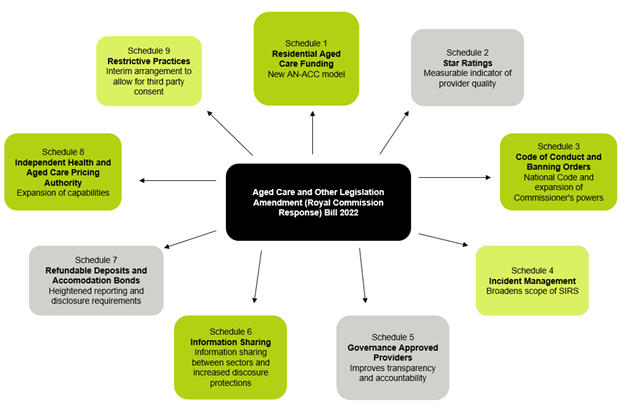
While we watch this space, we’ll set out the key components of the Royal Commission Response Bill and what the legislative changes mean for those in the industry.
Residential aged care funding
A new funding model for the calculation of residential aged care subsidies is being introduced: the new Australian National Aged Care Classification (AN-ACC) model will replace the antiquated Aged Care Funding Instrument (ACFI).
While the ACFI allowed providers to perform their own assessments of individuals, and subsequently allocates funding based on fixed rates accounted for by the individuals’ categorisation, the new AN-ACC model will require standardised assessments done independently of the service provider. The AN-ACC model adopts a two-pronged approach to funding, utilising:
- a variable subsidy per resident per day based on their AN-ACC classification; and
- an additional fixed subsidy dependent upon the characteristics of the aged care service.
The value of the second component remains somewhat flexible, with increased subsidies payable to those services operating in remote locations or providing specialist services, accounting for increased operating costs.
Star ratings system
The Royal Commission Response Bill aims to implement an information-sharing platform, by way of a star ratings system, allowing those within in the aged care system to make informed decisions about providers.
The number of stars allocated to a provider is based on measurable indicators of quality and is ultimately reflective of the standard and safety of the service provided. The system will indicate an overall star rating for each service provider, as well as communicating the standard of the provider’s performance in sub-categories focusing on quality indicators, service compliance ratings, consumer experience, and staff care minutes.
The star ratings themselves will be published by the Secretary of the Department of Health and Aged Care to the My Aged Care website. To protect the integrity of the star ratings system, the Secretary will not be liable for civil proceedings in respect of any loss, damage or injury suffered by a service provider as a result of the publication of a star rating.
Code of conduct and banning orders
A new Code of Conduct will apply to providers and their employees within the aged care system. With the current Code implemented at a State and Territory level, the new Code will be enforced at a national level and will expand the power and functions of the Aged Care Quality and Safety Commissioner. It will be based on that of the current National Disability Insurance Scheme, with the intention being alignment of the obligations between both the care and support sector.
Under the new Code, the Commissioner will have the right to issue a banning order against current and former aged care workers and governing persons of approved providers, preventing them from operating in the aged care sector. Civil penalties will be imposed against employees, employers, and governing persons of approved providers found to be in breach of a banning order.
Incident management and reporting
The scope of the Serious Incident Response Scheme (SIRS) will be extended to cover providers of home care and flexible care delivered in a home or community setting, in addition to those providing traditional residential care. SIRS was introduced in 2021 in an attempt to reduce incidents of abuse in Government funded aged care residences. The Royal Commission Response Bill introduces new incident reporting responsibilities for a broader range of aged care providers. One of these responsibilities will include the implementation and maintenance of an incident management system compliant with the Quality of Care Principles 2014.
Governance-approved providers
New governance responsibilities aimed at improving transparency and accountability within the aged care system will apply to the membership of governing bodies of aged care providers, the establishment of new advisory bodies, and measures aimed at improving leadership and culture within the industry.
Aged care providers will also bear the burden of providing information to the Department of Health and Aged Care Secretary each year, specifically in relation to their operations, in order to ultimately increase transparency for aged care recipients and their families.
Information-sharing between Commonwealth agencies
The Royal Commission Response Bill amends various pieces of legislation to further the ability of Commonwealth bodies within the aged care, disability and veterans’ affairs sectors to share information with respect to direct and indirect non-compliance with the New Code.
The Secretary’s powers now allow them to disclose protected information in situations where they believe a breach of professional standards may have occurred or be likely to occur. Previously, the Secretary’s power was more restrictive, with disclosure reliant upon their belief that conduct had already breached professional standards.
Use of refundable deposits and accommodation bonds
A three-phase plan to implement a new financial and prudential framework for the aged care sector is being implemented. The first phase, on the financial information of aged care service providers, introduced mandated reporting and heightened powers of information-collecting. The second phase, which is in this Bill, will amend the Aged Care Act to enable the Secretary or the Commissioner to request information or documents relating to a loan made using a refundable deposit or accommodation bond.
This amendment aims at protecting individuals’ refundable deposits, while holding providers accountable and ensuring the deposit process remains transparent for aged care residents and their families.
Independent Health and Aged Care Pricing Authority
The Royal Commission Response Bill expands the capabilities of the Independent Health and Aged Care Pricing Authority, formerly known as the Independent Hospital Pricing Authority. These will include the provision of advice on health and aged care pricing and costing matters and the performance of certain functions conferred in the Aged Care Act.
It will also establish the Aged Care Advisory Committee within the Pricing Authority, with its objective being supporting the Pricing Authority with its aged care pricing advice functions.
Restrictive practices
The final amendment proposed by the Royal Commission Response Bill is to strengthen the arrangements regarding the use of restrictive practices, specifically combatting unexpected outcomes in respect of the interactions with State and Territory guardianship and consent laws.
Restrictive practices refer to actions that restrict the rights or freedom of movement of an individual in receipt of care. If the care recipient is unable to provide consent themselves, it must be received from a person who can give consent under the relevant State or Territory law. Unexpected complications arose upon the introduction of this requirement in 2021, so the Bill introduces interim arrangements to address this issue until State and Territory laws are amended accordingly.
The amendment would allow the Quality of Care Principles 2014 to make further provision for the giving of informed consent where the care recipient does not have the capacity to consent themselves. This would include the authorisation of an individual to provide consent on the care recipient’s behalf. The amendments would also provide for an immunity provision which would protect providers reliant upon the consent given by a substitute decision-maker in situations involving restrictive practices.
Further reform
The Royal Commission Response Bill is just one element of the current Government’s plan to reform the aged care system in Australia.
Labor’s Aged Care Amendment (Implementing Care Reform) Bill 2022 is currently before Parliament. This second Bill attempts to make three further key changes to the Australian aged care system. The Bill creates a new responsibility for aged and residential care providers (as well as certain flexible care providers) to always have a registered nurse on site, across all facilities that they operate. Secondly, the Bill empowers the Government to put a cap on fees charged by providers of home care, as well as remove the providers’ ability to charge exit fees. Finally, the Bill requires the Secretary of the Department of Health and Aged Care to publish information relating to aged care services, ultimately increasing transparency and accountability within the system.
Other than the two Bills, the current Government has yet to date announced any further steps that they are willing to take in order to implement the remaining recommendations of the Royal Commission. As this second Bill progresses through Parliament we will continue to provide further updates and insights, but in the meantime we are left to watch this space!
Get in touch